Prague Proton Therapy Center and the COVID-19 Crisis - Delivering Cancer Treatment During Challenging Times
29. 1. 2021 14:27The COVID-19 pandemic has had a massive impact upon health care systems all over the world, hindering cancer diagnoses for millions of patients, and slowing the progress of advanced innovations in care that could improve the lives of future generations.
During these challenging times, the Proton Therapy Center in Prague continues to treat cancer patients from many countries, giving hope to cancer sufferers that may otherwise be unable to access such advanced treatment in their home countries.
Proton Therapy Center in Prague Adapts to the New Normal
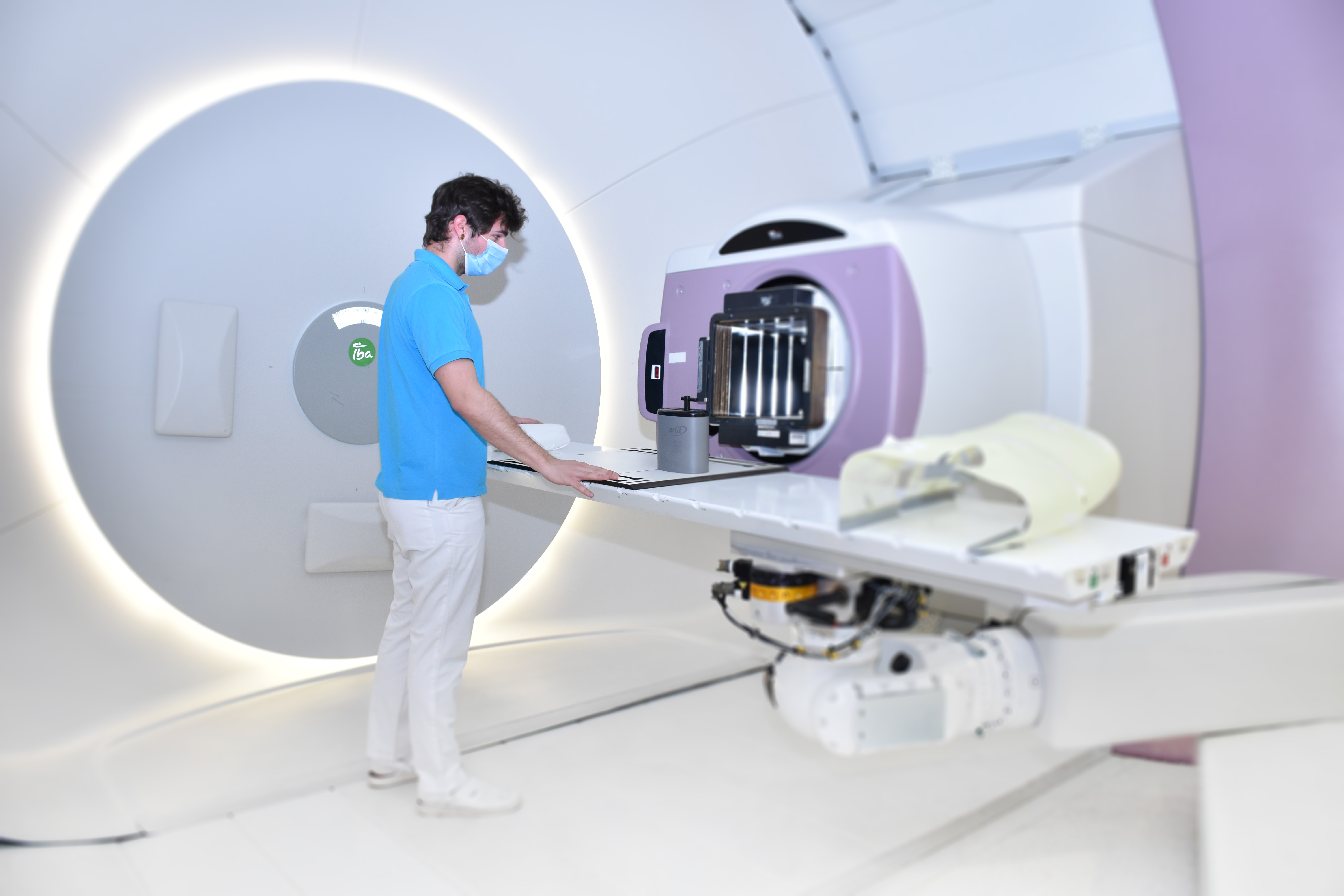
Operating a state-of-the-art proton therapy facility in Prague during and after the peak of the COVID-19 crisis in Europe has forced its treatment team to be flexible in response to the unprecedented challenge of the COVID-19 world-wide pandemic.
With the implementation of strict safety protocols and adaptations for patients and staff, our team at the Proton Therapy Center has successfully maintained continuous treatment throughout the pandemic.
To ensure that success, we have instituted many safety precautions, including daily screenings of every staff member, patient, and visitor to the centre; strict enforcement of mask wearing, social distancing, and hand sanitizing; limiting visitors; and frequent alcohol-based cleanings of all treatment and public areas throughout the building.
Our team has also increased its telehealth platform use, in order to reduce the risk of in-person virus transmission. (The rise of telemedicine in fact will likely become one of the defining influences of the pandemic on health care around the world.)
At this time, we continue to be extremely vigilant – in order to create a safe treatment space for our vulnerable cancer patients. The health of our patients is always our top priority, and it remains our plan to keep every safeguard possible in place until the risk of infection finally abates.
The Benefits of Proton Therapy in Prague
Proton therapy has emerged as the most promising advancement for patients with a wide range of cancers.
Compared to traditional (photon) radiation, proton therapy enables more precise targeting of cancers, which results in fewer side effects and improved health outcomes. It has proven highly effective in treating difficult-to-target cancers such as paediatric, head & neck, brain, thoracic, gastrointestinal, and breast tumors.

Proton therapy has been demonstrated to have fewer side effects across many cancers compared to conventional radiotherapy, reducing costly side effects and hospitalisations during treatment. It has also been shown to lead to fewer secondary radiation-induced tumours and better preserves quality of life across several cancers compared with photon therapy.
Cancer survivors are living longer due to effective treatments, and it is more important than ever to preserve quality of life for long-term survivors.
Robust data have emerged over the past decade demonstrating the superiority of proton therapy across numerous individual cancer types. Compared with conventional radiotherapy, proton therapy can:
- improve overall survival and reduce high-grade complications for head and neck cancers;
- improve tumour control and survival for base of skull cancers and chordomas;
- reduce side effects for brain tumours;
- improve survival for both locally advanced and early-stage lung cancer;
- improve survival and reduce high-grade complications and costly hospitalisations for esophageal cancer,
- improve survival and reduce complications for hepatocellular carcinoma,
- reduce side effects for pancreatic and gastrointestinal tumors,
- lead to excellent long-term outcomes with fewer long-term side effects for prostate cancer;
- reduce acute and chronic lifelong side effects for pediatric cancers; and
- expand curative options for patients with recurring tumours.
You can send your medical documentation for assessment of the suitability of proton therapy by e-mail to patient@ptc.cz. Alternatively, you can contact our treatment coordinators, who are prepared to answer all of your questions related to proton therapy. You can call them at +420 222 999 000.
Sources:
Berman AT, Teo BK, Dolney D, Swisher‐McClure S, Shahnazi K, Both S,
et al. An in silico comparison of proton beam and IMRT for postoperative radiotherapy in completely resected stage IIIA non‐small cell lung cancer. Radiat Oncol. 2013;8:144.
Blanchard P, Gunn GB, Lin A, Foote RL, Lee NY, Frank SJ. Proton therapy for head and neck cancers. Semin Radiat Oncol. 2018;28:53–63.
Chang JY, Li H, Zhu XR, Liao Z, Zhao L, Liu A, et al. Clinical implementation of intensity modulated proton therapy for thoracic malignancies. Int J Radiat Oncol Biol Phys. 2014;90:809–18.
Colaco RJ, Hoppe BS, Flampouri S, McKibben BT, Henderson RH, Bryant C, et al. Rectal toxicity after proton therapy for prostate cancer: an analysis of outcomes of prospective studies conducted at the University of Florida Proton Therapy Institute. Int J Radiat Oncol Biol Phys. 2015;91:172–81.
Fagundes MA, Pankuch M, Hartsell W, Ward C, Fang LC, Cahlon O, McNee‐ ley S, et al. Cardiac‐sparing postmastectomy proton radiation therapy for women with stage III, loco‐regional, breast cancer: a dosimetric comparison study. Int J Radiat Oncol Biol Phys. 2013;87:S245.
Gomez DR, Chang JY. Accelerated dose escalation with proton beam therapy for non‐small cell lung cancer. J Thorac Dis. 2014;6:348–55.
Ho JC, Nguyen QN, Li H, Allen PK, Zhang X, Liao Z, et al. Reirradiation of thoracic cancers with intensity modulated proton therapy. Pract Radiat Oncol. 2018;8:58–65.
Hong TS, Wo JY, Yeap BY, Ben‐Josef E, McDonnell EI, Blaszkowsky LS,
et al. Multi‐Institutional phase II study of high‐dose hypofractionated proton beam therapy in patients with localized, unresectable hepatocellular carcinoma and intrahepatic cholangiocarcinoma. J Clin Oncol. 2016;34:460–8.
Huynh M, Marcu LG, Giles E, Short M, Matthews D, Bezak E. Current status of proton therapy outcome for paediatric cancers of the central nervous system—analysis of the published literature. Cancer Treat Rev. 2018;70:272–88.
Jakobi A, Bandurska‐Luque A, Stützer K, et al. Identification of patient benefit from proton therapy for advanced head and neck cancer patients based on individual and subgroup normal tissue complication probability analysis. Int J Radiat Oncol Biol Phys. 2015;92:1165–74.
Leroy R, Benahmed N, Hulstaert F, Van Damme N, De Ruysscher D. Proton therapy in children: a systematic review of clinical effectiveness in 15 pediatric cancers. Int J Radiat Oncol Biol Phys. 2016;95:267–78.
Phan J, Sio TT, Nguyen TP, Takiar V, Gunn GB, Garden AS, et al. Reirradiation of head and neck cancers with proton therapy: outcomes and analyses. Int J Radiat Oncol Biol Phys. 2016;96:30–41.
Takagi M, Demizu Y, Terashima K, Fujii O, Jin D, Niwa Y, et al. Long‐term outcomes in patients treated with proton therapy for localized prostate cancer. Cancer Med. 2017;6:2234–43.
Tai‐Ze Yuan, Ze‐Jiang Zhan, et al. New frontiers in proton therapy: applications in cancers. Cancer Comm. 2019; 39, 1-7.
Taylor CW, Kirby AM. Cardiac side‐effects from breast cancer radiotherapy. Clin Oncol (R Coll Radiol). 2015;27:621–9.
Toramatsu C, Katoh N, Shimizu S, Nihongi H, Matsuura T, Takao S, et al.
What is the appropriate size criterion for proton radiotherapy for hepatocellular carcinoma? A dosimetric comparison of spot‐scanning proton therapy versus intensity‐modulated radiation therapy. Radiat Oncol. 2013;8:48.
Waddle MR, Heckman M, Diehl NN, Stross W, Miller D, Kaleem T, Miller RC, May BC, Peterson JL, Vallow LA, Tzou KS. Survival after proton and photon radiation therapy in patients with head and neck cancers: a study of the national cancer database. Int J Radiat Oncol Biol Phys. 2018;100:1330.
